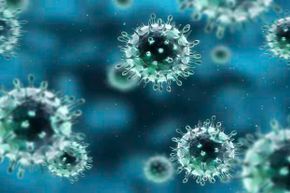
Millions of Americans get seasonal influenza, commonly called the flu, a contagious viral infection that attacks your respiratory system, including the nose, throat and lungs [source: Centers for Disease Control and Prevention].
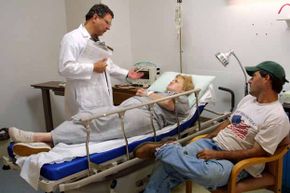
And the flu is nasty stuff. Each year, more than 200,000 Americans get so sick that they have to be hospitalized, and in a bad flu season, close to 50,000 people may die from flu-related illnesses [source: CDC]. Additionally, the flu costs the U.S. economy more than $10 billion in medical expenses and another $16 billion in lost earnings [source: Trust for America's Health].
Advertisement
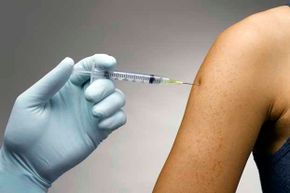
So you'd think that by now, we'd all have a pretty good understanding of the flu and what we need to do to deal with it. Well, guess again. Consider, for example, the prudence of getting an annual flu vaccine shot, a tried-and-true method of protecting yourself from the illness that the Centers for Disease Control and Prevention (CDC) now recommends for all Americans ages 6 months and older.
Amazingly, despite that recommendation, fewer than half of Americans go to the trouble of getting the injection, even though it's something that they can do at the local drugstore these days [source: Trust for America's Health].
Why are we so cavalier about our health? One part of the problem, as a 2010 Consumer Reports poll revealed, is that many of us either don't know much about the flu or have the facts dangerously wrong. For example, of the 30 percent of Americans who told pollsters they definitely wouldn't get a flu shot, 41 percent said they worried that flu vaccine was unsafe -- a belief that's been repeatedly refuted by health experts [source: Consumer Reports].
But with the flu, what you don't know can make you sick -- or even dead. To help you to avoid that fate, here are 10 of the most common misconceptions about the flu, along with the real facts.