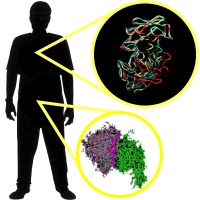
More than a century ago in Cameroon, around 1908 to be a bit more precise, a hunter brought down a chimpanzee with a well-aimed arrow. While gutting his kill, the hunter accidentally cut himself, bringing the chimp's blood directly into contact with his own. And in that moment, an unknown virus "spilled over." In other words, it jumped from one species to another. So begins the story of AIDS — perhaps.
The tale of the "cut hunter" is just a theory, but it's considered one of the most plausible scenarios for how a simian immunodeficiency virus jumped from chimps to humans and became HIV.
Advertisement
Remarkably, we do know for certain where the crossover happened because scientists can track it. Like all viruses, HIV mutates, and it does so at a constant rate. Scientists can use this rate of mutation to track the history and progress of the virus. Because of HIV's close resemblance to a simian immunodeficiency virus, researchers knew it must have originated as a virus carried by chimps. Through an exhaustive process of taking chimp stool samples all over Africa and measuring the rate of mutation in the viruses they found, scientists narrowed down the location of "spillover" to a remote corner of present-day Cameroon in the early 20th century.
What likely happened next is that the injured hunter traveled downriver to a nearby town where he unwittingly infected somebody else through sexual contact. The virus would then have worked its way from town to town until it reached Leopoldville, now Kinshasa, capital of the Democratic Republic of Congo. As Kinshasa's population exploded between the 1920s and the 1950s, Belgian colonial officials were conducting medical treatment campaigns that involved multiple injections with reusable syringes. This would have spread the virus more rapidly.
In 1960, the Belgians abandoned the Congo, and the Haitians who made up the bulk of Kinshasa's medical community returned to Haiti. At least one of them took HIV back with them. There, an American-run clinic was paying for blood plasma donations. The clinic's reusable needles helped spread the disease through Port-au-Prince, and, around 1969, some of that infected blood plasma made its way to the U.S. for use in hospitals or clinics. Once there, it spread among drug users via shared needles and among gay men via sexual contact [source: Lynch].
The virus, later named human immunodeficiency virus (HIV), causes the virulent condition known as auto-immune deficiency syndrome (AIDS). As of 2017, an estimated 35 million people have died of AIDS worldwide [source: WHO]. However, thanks to improved therapies and preventive measures, the number of deaths and new infections has declined steeply since peaking in 2005.
Advertisement