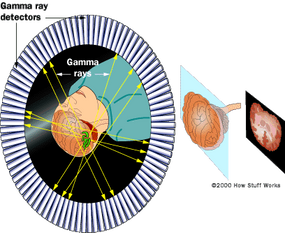
In hospitals or on TV, you've probably seen patients undergoing radiation therapy for cancer, and doctors ordering PET scans to diagnose patients. These are part of the medical specialty called nuclear medicine. Nuclear medicine uses radioactive substances to image the body and treat disease. It looks at both the physiology (functioning) and the anatomy of the body in establishing diagnosis and treatment.
In this article, we will explain some of the techniques and terms used in nuclear medicine. You'll learn how radiation helps doctors see deeper inside the human body than they ever could.
Advertisement
Imaging in Nuclear Medicine
One problem with the human body is that it is opaque, and looking inside is generally painful. In the past, exploratory surgery was one common way to look inside the body, but today doctors can use a huge array of non-invasive techniques. Some of these techniques include things like X-rays, MRI scanners, CAT scans, ultrasound and so on. Each of these techniques has advantages and disadvantages that make them useful for different conditions and different parts of the body.
Nuclear medicine imaging techniques give doctors another way to look inside the human body. The techniques combine the use of computers, detectors, and radioactive substances. These techniques include:
- Positron emission tomography (PET)
- Single photon emission computed tomography (SPECT)
- Cardiovascular imaging
- Bone scanning
All of these techniques use different properties of radioactive elements to create an image. See How Radioactivity Works for complete details.
Nuclear medicine imaging is useful for detecting:
- tumors
- aneurysms (weak spots in blood vessel walls)
- irregular or inadequate blood flow to various tissues
- blood cell disorders and inadequate functioning of organs, such as thyroid and pulmonary function deficiencies.
The use of any specific test, or combination of tests, depends upon the patient's symptoms and the disease being diagnosed.
Advertisement