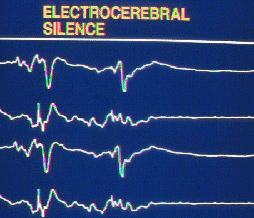
Confirming Brain Death
Many physicians request additional, confirmatory tests before pronouncing brain death. The two most common are the electroencephalogram (EEG) and the cerebral blood flow (CBF) study.
The EEG measures brain voltage in microvolts. It is so sensitive that the static electricity in a person's clothes will give a squiggle on the EEG (a false positive). All positive responses suggest brain function. The patient in the deepest coma will show some EEG electroactivity, while the brain-dead patient will not.
Advertisement
The cerebral blood flow (CBF) study study involves the injection of a mild radioactive isotope into the blood stream. By placing a radioactivity counter over the head, one can measure the amount of blood flow into the brain. (See How Nuclear Medicine Works.) The cerebral blood flow study takes 20 to 30 minutes to perform. If there is no blood flow to the brain as demonstrated by this study, the brain is dead. A negative cerebral flow study is indisputable evidence of a dead brain.

Another confirmatory test is chemical: The patient can be given 1 mg of atropine IV. In the patient with an intact brain, atropine will dramatically increase the patient's heart rate. In a brain-dead patient, atropine will not influence heart rate.
Now you have some idea of the scope of the examination that takes place before a patient is pronounced "brain dead." Patients are considered either alive or dead. One cannot be "almost" brain dead or "essentially" brain dead. Brain death, like pregnancy, is either "yes" or "no." Likewise, brain death is a very conservative diagnosis. It is not made lightly, but only when there is no doubt in the findings.
The criterion for the determination of death has always been left to physicians. The diagnosis of "brain death" is only possible because of modern medicine's ability to maintain the functions of supporting organs of the body after the brain is no longer viable. This support of the body is essential to evaluate the patient for possible survival and returning function of the brain. Once the examination of the brain has determined that it is no longer viable and there is no chance of any recovery of function, the "brain death" diagnosis is made.
Once a patient fulfills this medical criterion, nothing can be done for the patient. The patient can still be maintained physiologically on the ventilator, but there is no hope of any kind of recovery, even to a state of irreversible coma.
The brain performs many functions, including thought, movement and all the neurological function that allow the body to maintain blood pressure, heart rate, body temperature and organ function. When the brain dies, the body's organs will collapse. Massive artificial medical measures must be started to maintain organ function, but even in the best hands, these interventions are only a temporary measure.
Families of a brain dead patient must, by federal regulations, be provided the option of organ donation. If the family consents, the regional organ procurement organization is involved. If the family refuses, the mechanical ventilator, medications and fluids are discontinued, after which the heart stops.