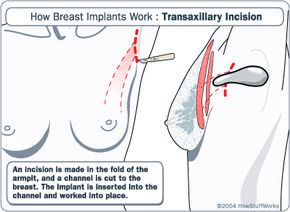
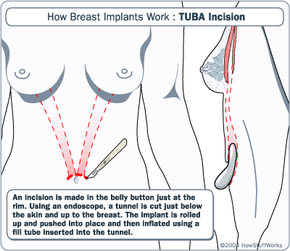
As with all surgeries, there are risk associated with breast augmentation. First and foremost, there is the risk of infection. Unusually high fevers are generally an indication of infection after surgery, and patients should watch for this after any invasive medical procedure.
Let's go over some of the risks specific to implant surgery.
Bottoming Out
This is the effect created when the implant sits too low and the nipple rides to high. This creates an unnatural look that is the result of cutting too large a pocket for the implant. It can also be caused by the weight of the implant in thin-skinned women. This is correctable with additional surgery.
Capsule Contracture
Capsular contracture is not a risk or complication in the traditional sense: It is definitely going to happen to a certain degree. It's the amount of contracture that is the issue. Capsule contracture causes the implant to be squeezed by the fibrous scar tissue that forms around it. The result can be a painful hardening of the breasts. This is the most common complication of breast-augmentation surgery. It is dealt with in a revision surgery where the scar tissue is scraped out to make more room for the implant. It can sometimes take several of these surgeries to correct the problem.
Hematoma
This is a common surgical risk that is caused by blood pooling under the skin. It can create discolored, possibly painful lumps. This can be corrected with surgery or drainage.
Interference with Mammography
The saline or silicone in breast implants can obscure X-ray results and hide potentially cancerous growths. Submuscular is the best placement to reduce this risk. It is important that the radiologist knows the patient has implants when performing a mammography, as there are techniques that can be used to help work around them.
Necrosis
Necrosis or "tissue death" is a rare and serious complication. Dead tissue can form around the implant and prevent healing. This has to be dealt with by surgery or complete removal of the implant. Necrosis usually leaves large, permanent scars.
Rupture
While women with breast implants can participate in a variety of activities without fear, they must be mindful that their implants are not indestructible. Most breast implants come with a lifetime manufacturer's warranty that covers operational failure. But many things that cause implants to rupture are not covered by warranty, and some things (like certain surgeries and over- or under-filling) will actually void the warranty.
Seroma
Seroma is a collection of fluid around the implant. This minor problem is handled by draining the fluid with a needle.
Symmastia
Symmastia is one of the rarest risks -- it is the result of a surgical mistake that causes the implants to lift off the sternum. The result is one large breast across the front of the body, with no cleavage. This complication is hard to repair.
Traction Rippling
This occurs when a textured implant settles into place after the swelling has gone down. As the implant drops, it pulls on the scar tissue, which pulls on the skin. The result is a rippling in the breast. Only the use of smooth implants eliminates this risk.
Breast augmentation is one of the most common types of plastic surgery today. As with all surgeries (especially elective ones), it is important to understand the risks involved. For the most current and detailed information on all of the risks associated with breast augmentation, consult a qualified physician.
In the next section, we'll learn how men use plastic surgery to enhance their chests.